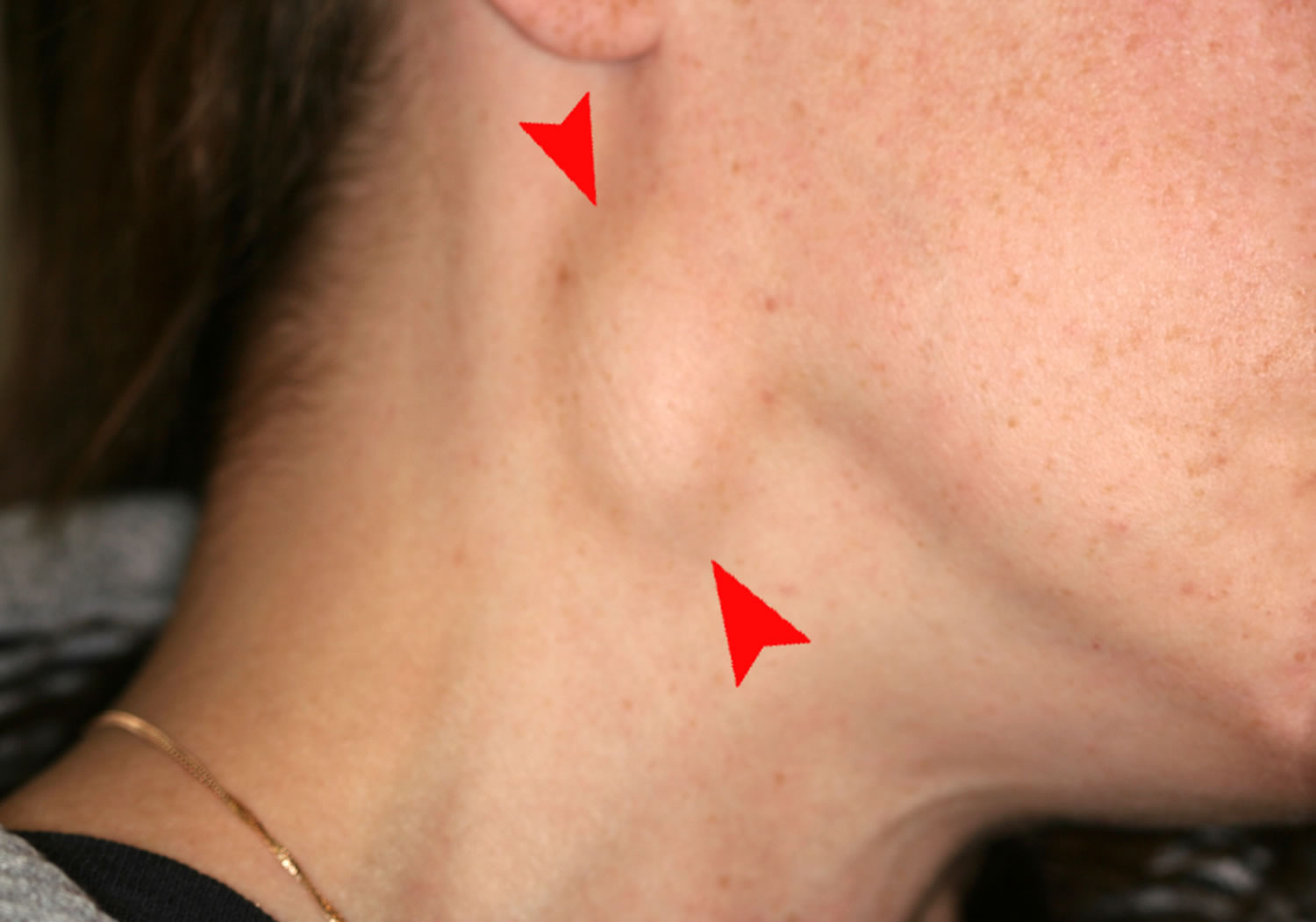 
Īfter a history and physical examination are completed, lymphadenopathy is placed into 3 categories:Ĭonsumption of under-cooked food/untreated water Īlthough there is no "cookbook" for the laboratory evaluation of generalized unexplained lymphadenopathy, the initial steps are to obtain a complete blood count (CBC) with a manual differential and EBV serology. If non-diagnostic, the next steps would be PPD placement, RPR, chest x-ray, ANA, hepatitis B surface antigen, and HIV test. The use of these cues and selection of the correct arm of the algorithm allows for a fairly rapid and cost-effective diagnosis of lymphadenopathy, including determination when it is safe to observe. It also is accepted that all generalized lymphadenopathy merits clinical evaluation, and the presence of "matted lymphadenopathy" is strongly indicative of significant pathology.Examination of the patient's history, physical examination, and the demographic in which they fall can allow the patient to be placed into 1 of several different accepted algorithms for workup of lymphadenopathy. Generally, the majority of the lymphadenopathy is localized (some site a 3:1 ratio), with the majority of that being represented in the head and neck region (again, some site a 3:1 ratio). In contrast, a person with generalized lymphadenopathy and fatigue would require more extensive investigation. For example, a patient with posterior cervical adenopathy, sore throat, and tremendous fatigue need only a careful history, cursory examination, and a mono test. The extent of the history and physical is determined by the clinical presentation of the patient. Additionally, the demographic particulars of the patient, including age, gender, exposure to infectious disease, toxins, medications, and their habits, may provide further cues.Īs evidenced above, the critical step in evaluation for adenopathy is a careful history and focused physical exam. A thorough history of any prodromal illness, fever, chills, night sweats, weight loss, and localizing symptoms can be very revealing. The nodes themselves may be tender or non-tender, fixed or mobile, discreet or "matted" together. Concomitant symptomatology and the epidemiology of the patient and the illness provide further diagnostic cues. Lymph nodes are distributed in discrete anatomical areas, and their enlargement reflects the lymphatic drainage of their location. Localized adenopathy occurs in contiguous groupings of lymph nodes. Generalized lymphadenopathy entails lymphadenopathy in 2 or more non-contiguous locations. Lymphadenopathy occurs in 2 patterns: generalized and localized. The pattern, distribution, and quality of the lymphadenopathy can provide much clinical information in the diagnostic process. However, an epitrochlear node of above 0.5 cm is deemed to be pathological in an adult. For example, children younger than ten have more hypertrophic immune systems, and nodes up to 2 cm can be considered normal in some clinical situations. However, the reality is that "normal" and "enlarged" criteria vary depending on the location of the node and the age of the patient. It is generally held that a node size is considered enlarged when it is more significant than 1 cm. In this reaction, there is some multiplication of the responding resistant cell line, and thus, the node itself increases in size. In this way, the immune system can recognize and react to foreign proteins and mount an immune response or sequester these proteins as appropriate. It consists of a multi-layered sinus that sequentially exposes B-cell lymphocytes, T-cell lymphocytes, and macrophages to an afferent extracellular fluid. The lymph node functions as an antigen filter for the reticuloendothelial (RE) system of the body. A clear understanding of lymph node function, location, description, and the etiologies of their enlargement is important in the clinical decisions of which cases need rapid and aggressive workup and which need only be observed. However, it is generally recognized that most lymphadenopathy, both localized and generalized, is of benign, self-limited etiology. Patients and physicians have varying degrees of associated anxiety with the finding of lymphadenopathy as a small number of cases can be caused by neoplasm or infections of consequence, for example, HIV or tuberculosis (TB). Lymphadenopathy is a common abnormal finding during the physical exam in general medical practice.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
